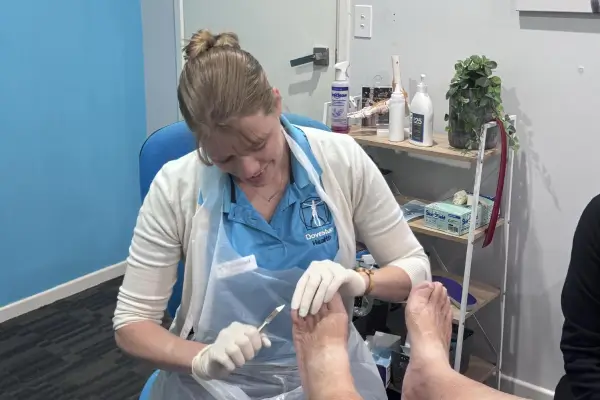
What is an NDIS Diabetes Educator?
We recognised that diabetes is usually medically treated but there are many people with disabilities who find it difficult to manage diabetes due to limitations. Our Credentialled Diabetes Educator (CDE) is able to make diabetes management easier by tailoring tools, education and skills to suit an individual’s needs and ensure they remain independent without compromising their health.
How can we help our NDIS Participants?
Our diabetes educator focuses on not only assisting the participant but also training carers and family in managing diabetes whether it be; blood glucose monitoring; insulin injection techniques; adjusting to life with diabetes; understanding carbohydrates (portions, type and timing); lifestyle and sick day impacts of diabetes; mental health and managing diabetes; diabetes and driving; annual cycle of care; diabetes related complications and travel.
Participant Success Story
Gregory, aged 45, has a mild intellectual disability and sensory impairment that effects his vision, he lives alone and has carers a few times a week. He came to see the diabetes educator as his GP said he needs to better manage his blood glucose levels (BGL) as he has Type 2 Diabetes (T2DM). His HbA1c was 9.2% and the GP recommended to start insulin, which Gregory did not want to do. Gregory thought he was struggling to manage his blood glucose levels because he always found it difficult to use a blood glucose monitor due to his disabilities and he didn’t like to prick his fingers. Gregory was reluctant to commence insulin and wanted more guidance on how to manage T2DM while staying independent. The diabetes educator discussed target ranges for blood glucose level and stated the goal for HbA1c is less then 7%. To assist with monitoring BGL the diabetes educator applied a continuous blood glucose monitor to Gregory’s arm which he could then use his phone to record the readings. This made it easy for Gregory to see on his phone as it was zoomed in and the app allowed him to set reminders. He could also record his food and activity level which he found it very easy to do and he could share information about what his BGL’s were doing through the app with carers and family. Gregory was able to get his HbA1c to 7.7% within 3 months as he learnt more about what his BGL are doing during his daily activities and which foods effect his BGL’s. Gregory felt he had more control as he learnt about T2DM in a way he could understand by speaking with the diabetes educator who tailored tools and a treatment plan.